Long-term health planning often gets discussed as something people should think about someday, usually after a concern becomes unavoidable. In reality, the most effective health planning happens well before urgency enters the picture. Early clarity gives individuals a way to understand where they stand, what may need attention, and how to move forward without rushing into decisions that feel reactive or incomplete.
What has changed in recent years is how much information is available and how quickly it can influence care paths. Tests, referrals, and treatment options now appear early in the process, sometimes before people feel ready to interpret them. Without clarity at the start, long-term planning can feel fragmented. With it, health decisions become more deliberate, less stressful, and easier to revisit as circumstances change.
Early Insight
Identifying health concerns early provides a comprehensive roadmap for long-term care decisions. Instead of guessing based on symptoms alone, individuals gain a more complete internal picture that helps guide next steps. This early insight creates context, making it easier to understand whether a concern requires immediate attention, monitoring, or simple lifestyle adjustments.
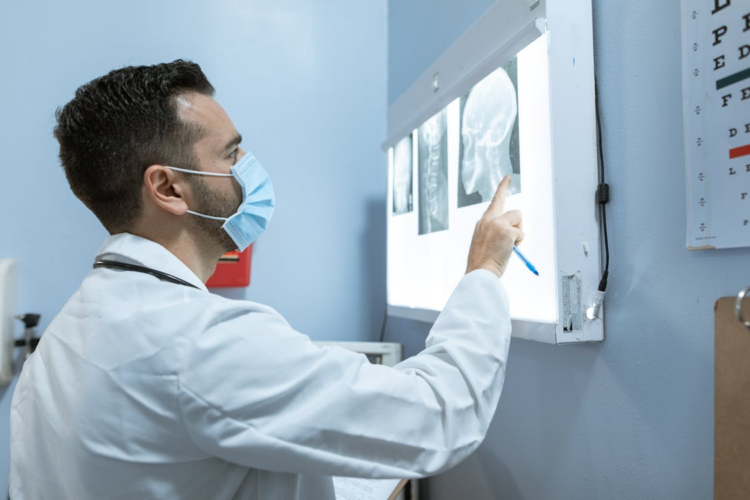
When diagnostic imaging solutions are part of this early stage, they add depth to this understanding. Providers can reference concrete data rather than assumptions, and patients gain confidence in what is being discussed. Organizations such as Numed support this process by helping ensure imaging results are timely and effectively communicated, allowing early clarity to shape care plans rather than complicate them.
Baseline View
Clear baseline information plays a quiet but critical role in long-term health planning. A baseline offers a reference point that future changes can be measured against, which is especially important for conditions that develop gradually. Without that starting snapshot, it becomes harder to tell whether a change is meaningful or simply part of a normal range.
Having baseline data also changes how people engage with their health over time. Follow-up visits become more focused. Monitoring feels purposeful rather than vague. Patients and providers can look at trends instead of isolated results, which supports decisions that are steady and informed rather than rushed.
Treatment Confidence
Uncertainty often shapes how people experience treatment discussions. When information feels incomplete or unclear, conversations can feel overwhelming, even when options are reasonable. Early clarity reduces that uncertainty by giving everyone involved a shared understanding of what is known and what still needs observation.
With clearer information on the table, treatment conversations shift tone. Questions become more specific. Decisions feel collaborative rather than imposed. Patients are better positioned to weigh options, understand recommendations, and participate actively in planning rather than simply reacting to them.
Goal Alignment
Timely insights help align care goals with realistic outcomes. Long-term health planning works best when goals are grounded in accurate information rather than assumptions or fear. Early clarity allows individuals to set expectations that reflect their actual situation, not worst-case scenarios or vague reassurance.
This alignment supports consistency. Care plans remain stable because they are built on understanding rather than urgency. Adjustments can still happen, but they happen with intention. This steadiness is especially valuable for managing chronic concerns or conditions that require periodic reassessment.
Fewer Interventions
One of the often-overlooked benefits of early clarity is its ability to reduce unnecessary interventions later. When concerns are identified and understood early, providers can distinguish between situations that require action and those that benefit from observation. As such, this prevents a cascade of tests or procedures driven more by uncertainty than need.
Clear early information supports restraint where appropriate. It allows care teams to avoid overcorrection while still staying attentive. For patients, this translates into fewer disruptions, lower stress, and greater trust in the overall care process.
Reduced Stress
Uncertainty carries a unique weight in health planning. When people lack clear information, even routine decisions can feel heavy. Questions linger. Small symptoms feel larger than they are. The mind fills gaps with speculation, which often increases stress more than the situation itself.
Clear diagnostic information helps relieve that mental burden. Knowing what is happening, or just as importantly, what is not happening, allows people to breathe a little easier. Stress does not disappear, but it becomes manageable. Health planning moves from worry-driven reactions to measured consideration, which supports steadier emotional well-being over time.
Preventive Focus
Early clarity creates space for prevention that feels purposeful rather than generic. Without clear insight, preventive strategies often remain broad and unspecific. People hear general advice but struggle to connect it to their own situation.
When clarity exists early, prevention becomes targeted. Individuals understand why certain strategies matter and how they connect to their long-term outlook. This understanding improves follow-through. Preventive steps feel relevant rather than abstract, which increases consistency and engagement over the long term.
Faster Response
Clear early data helps avoid delays when new concerns emerge. Without a reference point, it can be difficult to determine whether a change requires attention or simply observation. Besides, uncertainty often leads to hesitation, which can slow response times.
Once early clarity is in place, changes stand out more clearly. Providers and patients can act with confidence, knowing decisions are based on comparison rather than guesswork. Faster responses do not necessarily mean aggressive action. They mean timely, appropriate action guided by context.
Ongoing Monitoring
Long-term health planning is rarely static. Conditions evolve. Bodies change. Early insights guide how monitoring should happen over time, helping avoid both neglect and over-surveillance.
With a clear starting point, monitoring strategies feel intentional. Follow-ups occur for specific reasons. Results are easier to interpret. Monitoring becomes a supportive tool rather than a source of anxiety, reinforcing continuity instead of disruption.
Better Dialogue
Communication improves significantly when early understanding exists. Patients with clearer insight ask more focused questions. Providers can explain recommendations with greater precision. Conversations feel collaborative rather than one-sided.
This shared understanding strengthens trust. Patients feel included in planning rather than spoken to. Providers can tailor guidance more effectively. Over time, this dialogue becomes one of the most valuable aspects of long-term health planning, supporting decisions that evolve without confusion or frustration.
Early clarity matters because it shapes everything that follows. It influences how decisions are made, how stress is managed, and how confidently people move through their health journey. Long-term planning built on understanding feels steadier, more flexible, and easier to maintain. Rather than reacting to uncertainty, individuals with early clarity engage with their health proactively. They monitor thoughtfully, communicate effectively, and adjust plans with intention. In a healthcare landscape that moves quickly and offers many choices, clarity at the beginning remains one of the strongest foundations for long-term health stability.